 |
Management
of the HBsAg Positive Patient
This article is reprinted with permission of the Hepatitis
B Coalition.
Introduction
The hepatitis B virus (HBV) is a DNA virus and a member of the hepadna
family of viruses, and is a very common virus with an estimated 300 million
carriers worldwide. Only 1 - 1.5 million of these are in the United States.
Hepatitis B is much more prevalent in other areas of the world such as
parts of Asia including Southeast Asia, sub-Saharan Africa, and some of
the Mediterranean countries. It is in these areas that hepatitis B-induced
liver cell cancer is such a common problem.
In those populations where hepatitis B is endemic, the virus is usually
transmitted from the infected mother to her child during the birth process
or sometimes between children, especially in areas where overcrowding
is common.
This is in contrast to the situation in Western countries where infection
is most often spread by the parenteral route, e.g., from needle stick,
or by sexual contact. Thus in these areas, infection usually occurs in
young adults. Because failure to clear the virus and development of chronicity
is much more common in those infected at a very young age, chronic hepatitis
B is much less common in Western countries than in areas where hepatitis
B is endemic.
Serologic Data
The hepatitis B virus is a complex virus with a central core and a protein
coat. A number of antigens are associated with this virus and each antigen
may result in the production of a corresponding antibody. Some of these
antigens and antibodies are detected in routine commercially available
assays. Assays to detect the hepatitis B virus DNA are now also available.
When the hepatitis B virus infects the liver, it replicates and produces
excess surface material, some of which reaches the blood. Only
when there is a great deal of viral replication does a significant load
of the virus reach the blood. When there is less viral replication, the
virus core is only detected in the liver but not in the blood (when
assayed by the routine commercially available tests). The marker for the
surface is HBsAg (hepatitis B surface antigen) and the markers for the
core are HBeAg (hepatitis B "e" antigen) and HBV-DNA.
There is a recently described mutant strain of HBV (pre-core mutant) in
which the virus cannot manufacture HBeAg and thus the only marker for
the presence of the virus core is HBV-DNA. These patients may have antibodies
to HBeAg and often have very severe liver disease.
| MARKER |
USUAL SIGNIFICANCE |
| HBsAg |
Virus is present |
| Anti-HBs (surface antibody) |
Virus is usually cleared
Patient immune |
| HBeAg* |
Active viral replication
Ongoing liver disease
Patient infectious |
| Anti-HBe* |
Viral replication reduced
Inactive liver disease (usually)
Less infectious |
HBV-DNA
(by routine commercially available assays) |
Active viral replication
Ongoing liver disease
Patient infectious |
| HBcAg |
Never detectable in serum |
| Anti-HBc (core antibody) |
Patient has come into contact with hepatitis
B and may or may not still be infected with the virus
Does not signify immunity |
IgM anti-HBc
(by routine commercially available assays) |
Signifies recent contact with hepatitis
B |
| *except for pre-core mutant strains of HBV |
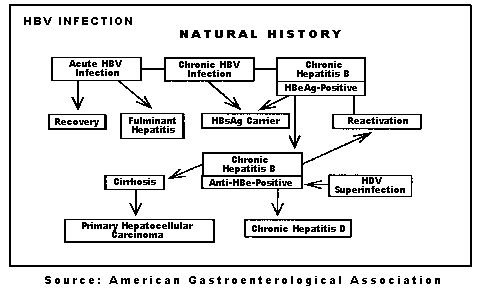
Natural History
Acute hepatitis B
When an individual is infected with hepatitis B virus, a typical acute
hepatitis can result. A significant number of cases produce a sub-clinical
and often unnoticed infection. Rarely (<1%) fulminant hepatitis may
develop and this has a very high mortality rate. These people are often
treated by urgent liver transplantation. Most people with an acute infection
test positive for HBsAg and IgM-antiHBc. After a variable period of time,
the HBsAg will disappear and anti-HBs will appear, signifying termination
of the infection.
The presence of hepatitis B surface antigen (HBsAg) signifies infection
with the virus but does not give any information concerning infectivity
or the presence of ongoing liver damage. When the virus is cleared from
an individual, the antibody to hepatitis B surface (anti-HBs) develops
and confers immunity to further virus infection. Anti-HBs often remains
for life.
The finding of hepatitis B "e" antigen (HBeAg), a marker of
the core of the virus, usually means that there is a great deal of viral
replication allowing the core to be present in the blood. The disappearance
of HBeAg and the appearance of an antibody to HBeAg usually means that
the level of viral replication and associated liver disease has lessened
and this individual is less capable of infecting others.
At some stage during the acute infection, HBeAg will be present but is
usually cleared as the virus replication and liver damage is reduced.
This disappearance may be followed by the transient appearance
of anti-HBe.
Hepatitis B core antigen (HBcAg) never appears freely in the blood. The
corresponding antibody (anti-HBc) appears in the blood at about the same
time as HBsAg and usually remains for life, even if HBsAg is cleared.
Anti-HBc does not imply immunity but merely signifies that the
individual has at some time been infected with the hepatitis B virus.
If the anti-HBc is of the IgM class of antibodies (as detected by routine
clinical assay) this signifies that the individual has recently been infected;
but if only the IgG antibody is detected, then the infection probably
occurred at least six months prior to the test.
Chronic hepatitis B
Most individuals infected with hepatitis B virus will clear the virus
with the development of anti-HBs. Only about five percent of people will
not clear HBsAg and will not develop anti-HBs. Anti-HBc will remain positive
in these patients. Those infected at a very young age are more likely
to develop chronic infection.
When an individual develops chronic hepatitis B, a variety of outcomes
are possible, ranging from a chronic carrier state with very little, if
any, liver damage to ongoing chronic hepatitis of varying degrees of severity.
The latter may at times progress to cirrhosis with all its clinical sequelae.
During the early phase of chronic infection, there is often significant
viral replication and ongoing liver damage as manifested by HBeAg positivity
and elevated transaminases. This often disappears after a variable period
of time although it may sometimes take some years for this to occur. When
the HBeAg does disappear, the liver disease becomes more quiescent and
the patient is less infectious. It is in this stage that the virus DNA
may become integrated into the host liver cell DNA. Hepatocellular carcinoma
may complicate long-standing chronic hepatitis B infection.
Even after the HBeAg has disappeared and the liver disease has become
relatively inactive, the whole process may be reactivated. Multiple cycles
of reactivation may occur. Episodes of reactivation may occur spontaneously
or may be precipitated by a course of immunosuppressant therapy (such
as steroids or chemotherapy given for an unrelated illness). Such an event
may result in worsening of the liver disease with a potentially severe
outcome. Thus, one has to watch closely any chronic hepatitis B carrier
who requires immunosuppressant therapy.
Management of HBsAg Positive
Patients
Patients who are HBsAg positive should be assessed as follows:
- Virologic and hepatic status
Clinical history (including family history) should be taken, in particular
looking for evidence of symptomatic liver disease in the patient, family,
or household member.
Physical examination to look for evidence of liver disease such as spider
nevi, jaundice, ascites, etc.
Biochemical tests to assess liver status (bilirubin, transaminases,
albumin, prothrombin time.) All of these should be repeated every six
months.
Anti-HBc IgM should be measured for evidence of recent (less than six
months) acquisition of the virus. This need only be done at initial
presentation and only repeated if positive.
HBeAg and/or HBV-DNA should be measured to assess if active viral replication
is present.
Individuals who have clinical and biochemical evidence of liver disease
should be further assessed and consideration given to liver biopsy.
In those with liver disease and active viral replication (HBeAg positivity)
treatment with interferon should be considered. This treatment is FDA-approved.
There are clinical trials underway involving other antivirals, e.g.,
lamivudine, which are showing promising results.
All HBsAg carriers should be monitored for the development of hepatocellular
carcinoma. Although there is much debate on the degree of frequency
of such monitoring and the modalities to be used, a reasonable approach
is to do ultrasound and alpha-fetoprotein estimation every six month,
especially if the infection has been present for ten years or more.
- Risks to others
Sexual contacts of any person acutely infected with hepatitis B are
at risk of acquiring hepatitis and should be vaccinated.
Family members of chronically infected persons (including non-sexual
contacts) are at risk of acquiring hepatitis B and, if not already infected
or immune, should be vaccinated. This approach should also be adopted
to newborn members of infected families, especially if the mother is
infected. In this latter case, hepatitis B immune globulin (HBIG) should
also be administered to provide immediate protection.
Conclusion
Hepatitis B virus infection is a complex virus which can produce a variety
of clinical situations. It can produce subclinical or clinical acute hepatitis
and it can go on to chronic hepatitis. This latter event is more common
when infection occurs at a very young age and is therefore more frequent
in areas of the world where the disease is highly prevalent and maternal-fetal
spread is common.
Chronic hepatitis infection can produce a range of sequelae, from very
little liver damage to chronic hepatitis varying from mild to more severe,
or even cirrhosis with all its complications. Hepatocellular carcinoma
is a risk of long-standing chronic hepatitis B infections.
This disease can now be prevented by vaccinating all at-risk persons.
There is also some new data suggesting that suitable patients with chronic
hepatitis B with significant liver damage and ongoing viral replication
may benefit from treatment with interferon. Trials of other antivirals
(e.g., lamivudine) are ongoing and appear to have promising results without
significant side effects.
What the Physician Can Do to Help
the Adult Hepatitis B Carrier
Coleman I. Smith, M.D.
Hepatologist
Minnesota Gastroenterology
Minneapolis, MN 55404
612-871-1145
- A YEARLY PHYSICAL to ensure the patient is healthy
without overt evidence of severe liver disease. This should include
evaluation of routine liver biochemistry (AST, ALT, alkaline phosphatase)
and liver function (bilirubin, albumin, prothrombin time) tests. Referral
to a specialist gastroenterologist/hepatologist if there is evidence
of deterioration in liver function.
- ALPHA-FETOPROTEIN (AFP)* every six months. The AFP
is a tumor marker which may become elevated when hepatocellular carcinoma
is present.
- AN ULTRASOUND OF THE LIVER* every six months. The
ultrasound may show small cancers in the liver before the blood abnormalities
develop and while the cancer is still treatable.
- HBsAg TESTING. HBsAg should be checked every year
to see if a person is still a carrier. Less than 1% of carriers clear
HBsAg and develop anti-HBs each year.
- HBeAg TESTING. If a person remains HBsAg positive,
HBeAg should be checked every year. This latter test will demonstrate
in most cases if the virus is actively replicating. A person who is
HBeAg positive (+) or has an AST>200 should be referred to a gastroenterologist/hepatologist
for evaluation of need for liver biopsy and anti-viral treatment. Indications
for referral include any of the following:
- HBeAg positivity
- ALT >200
- Deterioration in liver function
- Suspicion of a liver tumor
(The American Liver Foundation will provide names and phone numbers
of gastroenterologists and hepatologists in various regions of the
United States to whom patients may be referred. The phone number
is 800-223-0179.)
- TESTING OF HOUSEHOLD MEMBERS. All members of the
carrier's household and his/her sexual partners should be tested for
hepatitis B. If found susceptible or if they have an indeterminate pattern
(an isolated anti-HBc +) they should be vaccinated against hepatitis
B, even if pregnant.
- HEPATITIS B EDUCATION. Each hepatitis B carrier should
receive hepatitis B education, as should his/her household members and
sexual partners. Brochures to assist with education are available in
many languages and are free from the Hepatitis B Coalition, a program
of the Immunization Action Coalition. (See the address and phone number
below.)
* especially if infection has been present for over ten years.
Dr. Smith is a consultant gastroenterologist/hepatologist
at Minnesota Gastroenterology in Minneapolis. Smith has done extensive
research on hepatitis and is the author of dozens of publications. He
has written two articles for the Hepatitis B Coalition on the care of
the adult hepatitis B carrier. Additionally, Smith is a member of the
Advisory Board of the Hepatitis Coalition. This article is reprinted with
permission of the Hepatitis
B Coalition.
|

